In general, hip fractures refer to fractures (broken bone) of the part of the femur that is closest to the hip joint. All of the following are considered hip fractures: femoral neck fractures, intertrochanteric femur fractures, and subtrochanteric femur fractures. You may hear these terms used if you or a loved one ever sustains a hip fracture.
As the population continues to age, hip fractures are becoming increasingly common. In the older individual, they more commonly occur after a simple ground-level fall. Patients with poor bone quality (e.g. osteopenia or osteoporosis) are at highest risk of sustaining a hip fracture. As bone quality worsens as we age, older adults are therefore at the highest risk of a sustaining a hip fracture. Furthermore, mobility issues, which can be more common in the older adult, add to the risk of fracture as well.
Symptoms Associated with Hip Fractures
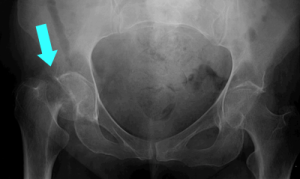 Hip fractures are quite painful. Usually if a patient has a hip fracture, he or she is unable to bear weight and may feel that they are unable to move the effected leg. Oftentimes, the leg appears short and the foot appears that it is rotated outwards. Simply, this position is the result of the pull of the muscles that exist around the hip on the fractured femur. Any time bones break, they bleed, and as such, hip fractures may be associated with bleeding into to the leg. With enough blood loss, the patient may feel confused, dizzy, or if severe enough, may even lose consciousness.
Hip fractures are quite painful. Usually if a patient has a hip fracture, he or she is unable to bear weight and may feel that they are unable to move the effected leg. Oftentimes, the leg appears short and the foot appears that it is rotated outwards. Simply, this position is the result of the pull of the muscles that exist around the hip on the fractured femur. Any time bones break, they bleed, and as such, hip fractures may be associated with bleeding into to the leg. With enough blood loss, the patient may feel confused, dizzy, or if severe enough, may even lose consciousness.
Diagnosis of Hip Fractures
The diagnosis of a hip fracture is often quite obvious as they are associated with severe pain and an inability to walk on the effected limb. Also, in the older population, they very commonly occur after a fall. If a hip fracture is suspected, you should have the patient brought to the nearest emergency department by ambulance for evaluation. A brief history and physical exam will be performed by the treating doctor. X-rays of the hip will then be ordered to confirm the diagnosis.
Treatment of Hip Fractures
The treatment for hip fracture in older adults most often involves surgery. Only in very rare situations (e.g. if the patient is normally bed-bound or very sick) is surgery not recommended. Surgery usually consists of two options: repair or replacement (arthroplasty). The decision for which surgical option is best depends mainly on the type of hip fracture that was sustained and the patient’s baseline mobility and health.
After surgery, patients normally stay in the hospital anywhere from 1 to 3 days depending on how well their pain is controlled and how well they are getting around with physical therapy. Oftentimes, longer-term physical therapy is needed to help the patient regain their mobility. The amount of therapy will depend on the patient’s underlying health status and how mobile the patient was before his or her injury. Depending on how much help the patient has at home (e.g. family, etc.) this may also include a short stay at a skilled nursing facility before the patient is able to return home.
Prevention of Hip Fractures
While sometimes hip fractures are inevitable, there are things that can be done to try to prevent them from happening. Fall prevention is a key factor. For instance, ask for help with daily tasks if your mobility has become limited and it is difficult for you to perform these without putting yourself at risk of falling. Remove loose rugs, repair loose flooring, and avoid placing electrical cords across walkways in your home. Using a non-slip mat in the tub and installing grab bars in the shower, tub, or next to your toilet may help with your balance and further decrease fall risk. In general, try to avoid slippery wet floors and avoid icy sidewalks during the winter months as much as possible.
Common Problems With Hips
- Osteoarthritis
- Dislocation (see image above of simple dislocation)
- Bursitis
- Fracture
- Femoroacetabular impingement
- Labral tear
- IT band syndrome
- Snapping hip syndrome
- Aseptic or Avascular necrosis
- Congenital Dislocation
- Acetabular dysplasia
- Coxa valga
- Coxa vara
- Tumor
- Legg-Perthes disease
