Renal System Anatomy
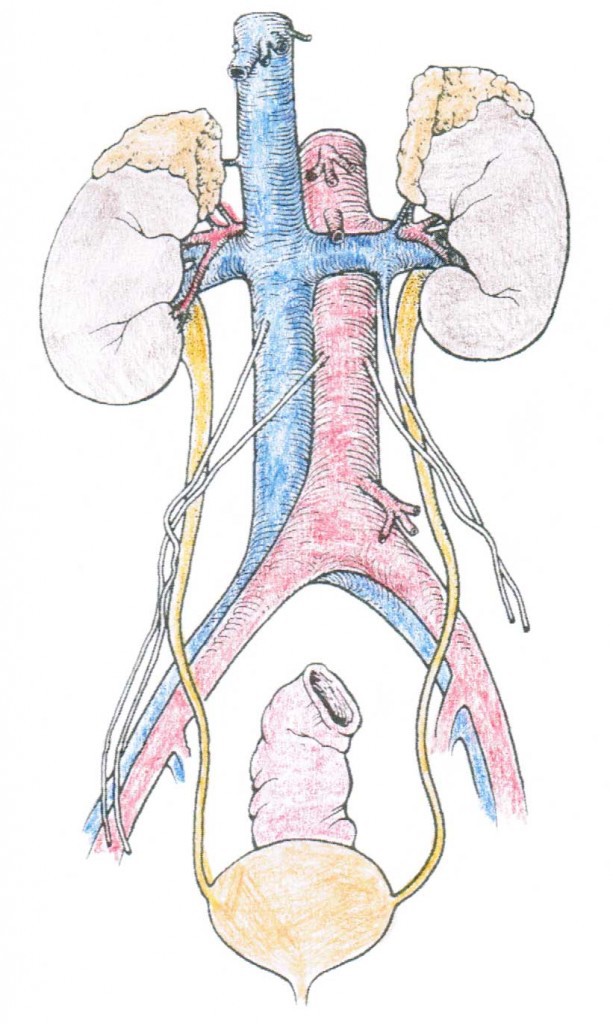
This image shows the kidneys, ureters, and bladder.
The bean-shaped kidneys are about the size of a closed fist. They lie against the back of the abdominal wall, outside the peritoneal cavity (which contains all of the bowels), just above the waistline in the lumbar (low back) region.
The adrenal glands (part of the endocrine system) sit on top of the kidneys and release a hormone called renin which helps to regulate blood pressure, and sodium (or salt) and water retention.
The right kidney often sits slightly lower than the left one because of the position of the liver. The kidneys are about 4 1/2 inches long and 2 1/2 inches wide. The kidneys are highly vascular (contain a lot of blood vessels) and are divided into three main regions: the renal cortex (outer region which contains about 1.25 million renal tubules), renal medulla (middle region which acts as a collecting chamber), and renal pelvis (inner region which receives urine through the major calyces).
The kidneys are protected in front by the contents of the abdomen and behind by the muscles attached to the spine. They are further protected by a layer of fat.
The Renal System
- Kidneys – Our body’s filtration system that collects waste products
- Ureters – Muscular tubes that transport urine from each kidney to the bladder.
- Urinary Bladder – A sac that collects and holds urine that comes from the ureters.
- Urethra – a narrow passageway where urine passes from the bladder to the outside of the body i.e. the process of urination.
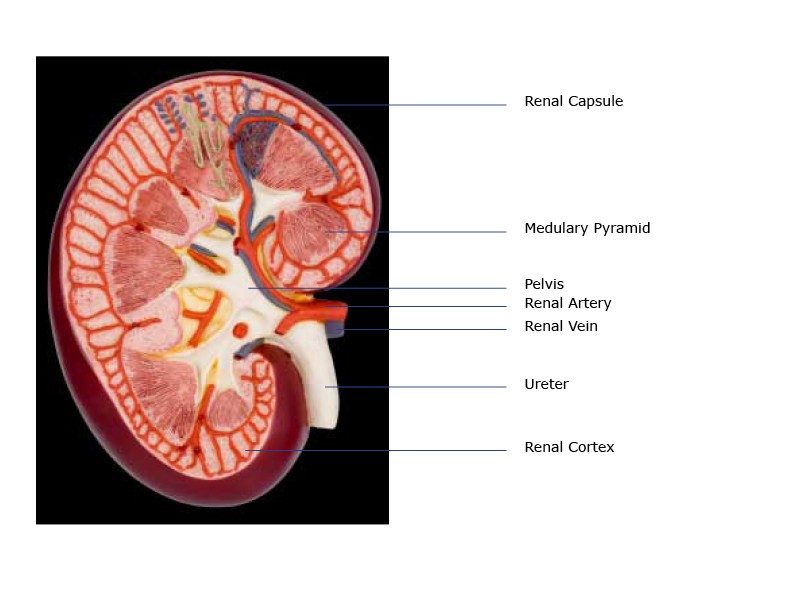
Kidney Anatomy
- Renal Capsule – An outer membrane that surrounds the kidney; it is thin but tough and fibrous
- Renal Pelvis – Basin-like area that collects urine from the nephrons (the kidney’s filtration system), it narrows into the upper end of the ureter
- Calyx – The extension of the renal pelvis; they channel urine from the pyramids to the renal pelvis
- Cortex – The outer region of the kidney; extensions of the cortical tissue, contains about one million blood filtering nephrons
- Nephron – these are the filtration units in the kidneys
- Medulla – the inner region of the kidney contains that contains 8-12 renal pyramids. The pyramids empty into the calyx.
- Medullary pyramids – Are formed by the collecting ducts, inner part of the kidney
- Ureter – Collects the filtrate and urine from the renal pelvis and transports it to the bladder
- Renal Arteries – A pair of arteries that branch off of the aorta bringing waste-filled blood into the kidney for filtering. Each minute, the kidneys receive 20% of the blood pumped by the heart.
- Renal Veins – Remove the filtered blood from the kidneys to the inferior vena cava
Kidney Function
Every minute, approximately 1300 mL of blood enter the kidneys, 1299 mL leave the kidney, and approximately 1 mL leaves the body as urine. The kidneys serve many functions. They maintain the balance of electrolytes, the acidity of the body, and overall fluid in the blood. This balance is maintained by the kidneys, no matter how much we eat or drink. If the body is dehydrated, the kidneys put less water is in the urine. When the blood becomes too acidic, the kidneys remove more acid from the blood and excrete in as urine. This is true of many electrolytes and other waste products.
As mentioned just prior, the kidneys remove waste products from the body (creatinine, urea, ammonia, etc.) while ensuring that essential substances are retained. The kidneys also produce the hormone erythropoietin that stimulates the production of red blood cells and enzymes.
The kidneys collect and get rid of waste from the body in 3 steps:
- Glomerular filtration – Filtrate is made as the blood is filtered through a collection of capillaries in the nephron called glomeruli.
- Tubular reabsorption – The tubules in the nephrons reabsorb the filtered blood in nearby blood vessels.
- Tubular secretion – The remaining filtrate which contains waste product passes through the tubules to the collecting ducts and is then taken to the bladder via the ureters.
The glomerular filtration rate (GFR) is the rate at which the glomeruli filter the blood. The normal GFR is 120 ml/minute. The most accurate measure of the GFR is done by measuring creatinine clearance. Clearance is the complete removal of a substance from the blood. Creatinine clearance is a good measure of filtration rate because creatinine (a waste product of the body) is filtered from the blood but is not reabsorbed by the tubules.
When the kidneys aren’t working as they should, as you might expect, this can lead to serious consequences. If the kidneys completely fail and this is not properly addressed, this can even lead to death. A Kidney Function Profile is used to test the health of the kidneys.
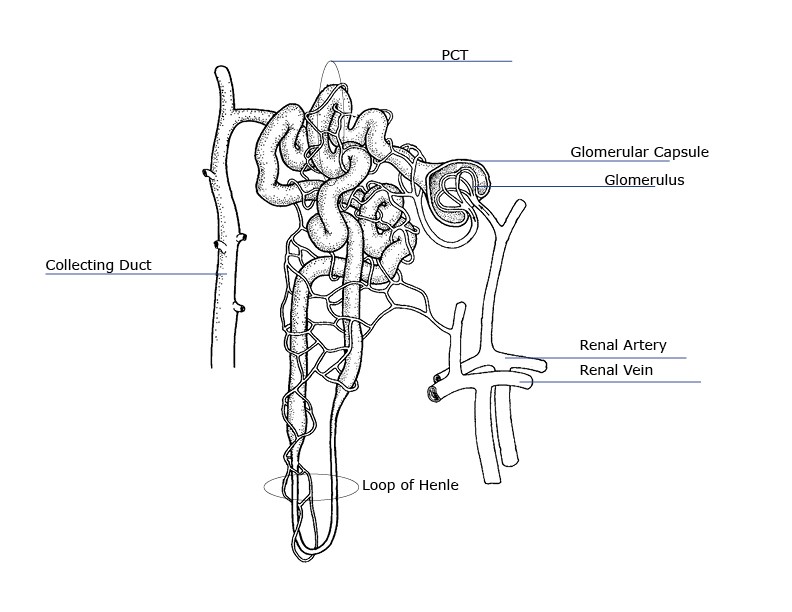
Nephron Anatomy
The nephron is the filtration unit of the kidney. It is the basic structural and functional unit of the kidney and cannot be seen by the naked eye. Each kidney has about 1 million nephrons. The walls of the nephron are made of a single layer of epithelial cells. Blood containing urea and metabolic waste products enters the kidney from the bloodstream. The blood is filtered by the kidney to remove wastes while leaving behind the blood cells and vital proteins and chemicals. The kidney also functions to help maintain body fluid and electrolyte homeostasis (balance).
- Renal Artery – brings waste-filled blood from the aorta to the kidney for filtering
- Arterioles – blood is brought to and carried away from the glomerular capillaries by two very small blood vessels—the afferent and efferent arterioles.
- Glomerulus – each glomerulus is a cluster of blood capillaries surrounded by a Bowman’s capsule. It looks similar to a ball of tangled yarn.
- Proximal convoluted tubule (PCT)
- Thin descending limb of the loop of Henle
- Thin Ascending limb of the loop of Henle
- Thick Ascending limb of the loop of Henle
- Distal convoluted tubule
- Renal Vein – when filtration is complete, blood leaves the nephron to join the renal vein, which removes the filtered blood from the kidney and delivers it back to the inferior vena cava
Nephron Function
- Glomerulus – Consists of a cluster of capillaries (small vessels)
- Proximal Convoluted Tubule – nearest the glomerulus; have permeable cell membranes that reabsorb vital metabolites and electrolytes into nearby capillaries.
- Loop of Henle – Has an ascending and descending limb, these loops function to reabsorb water. When the filtrate reaches the descending limb of the loop, water content has been reduced by 70%.
- Distal Convoluted Tubule – The farthest portion of the nephron from the glomerulus; helps to further regulate electrolyte homeostasis.
- Collecting Duct – collects the filtrate
Blood enters the kidney via the renal artery and goes to the glomeruli (plural for glomerulus). At each glomerulus, pressurized fluid leaks out of the blood stream through a filtration membrane. Large cells and proteins stay behind in the bloodstream. This creates a cell-free fluid (plasma) of water and small molecules that enters into the renal tubule. This plasma is taken to the nearest (proximal) convoluted tubule. This runs down into the loop of Henle and then back to the farthest (distal) convoluted tubule where many of the salts are reabsorbed back into the blood. The remaining fluid which contains waste products is transported down the ureters to the bladder where it is ultimately secreted as urine. (See Anatomy Terms to understand proximal and distal.)
What is urine made of?
Urine is made of water, urea, electrolytes, and other waste products. The exact contents of urine vary depending on how much fluid and salt you take in, your environment, and your health. Some medicines and drugs are also excreted in urine and can be found in the urine.
- 94% water
- 5% urea
- 1% sodium*
- .5% chloride*
- .25% potassium*
- .25% phosphate
- .25% sulfate
- .15% creatinine
- .1% uric acid
*Electrolytes
As mentioned prior, urine is formed in the nephrons by a three-step process: glomerular filtration, tubular reabsorption, and tubular secretion. The amount of urine varies based on fluid intake and one’s environment.
Kidney Disease and Disorders
Kidney diseases and kidney problems are usually treated by a nephrologist. Kidney stones are sometimes treated by a urologist. Here is a list of some of the more common kidney problems:
- Glomerulonephritis (nephritis) – inflammation of the glomeruli
- Hydronephrosis – excessive fluid within the kidney caused by blocked urine flow
- Pyelonephritis – infection of the kidney
- Kidney Stones (calculi) – usually form in the kidneys, but can form anywhere in the urinary tract
- Kidney Failure (acute and chronic)
- Kidney Tumors
- Kidney Cancer
- Nephrosis – a process that can lead to kidney failure
- Polycystic Kidney Disease – a disorder of the kidneys that result in multiple fluid-filled cysts within the kidney’s tissues
- Renal Hypertension – if the kidneys for some reason do not get enough blood, they set off a series of events leading to high blood pressure
- Renal Infarction – similar to a heart attack, but in the kidney, caused by blockage of kidney vessels
- Renal Vein clot – clot in the vein that carries blood from the kidney, can be fatal
Kidney Transplant
When dialysis fails to maintain the ideal kidney health and functioning, your doctor might recommend that you undergo a kidney transplant. These procedures are a last resort, and often allow an individual anywhere between 12 to 15 years of good health after the operation, depending on the source of the kidney.
According to the Centers for Disease Control and Prevention, there are over 100,000 Americans are on the waiting list for a kidney transplant. However, only 16,000 of these procedures are performed in a year. Another report stated that 4% of those who received a kidney from a deceased donor experience kidney failure within the first year after the transplant, while 21% of cases can take up to 5 years before any sort of complications arise. With that, the remaining 75% of transplants are relatively successful, albeit requiring significant maintenance and medication post-operatively.
Ultimately, the kidneys are an incredibly important set of organs that are essential for our health. If you believe you or a loved one have a kidney problem, please contact your doctor.
Of course, as always note that the information in this article is purely informative and should never be used in place of the advice of your treating physicians.