The goal of knee surgery is to get your knee working as close to a normal knee anatomy as possible. As with all major surgical procedures, complications can occur. The most common complications following knee replacement are:
- Thrombophlebitis
- Infection in the joint
- Stiffness of the joint
- Loosening of the joint
This is not intended to be a complete list of the possible complications, but these are the most common.
Thrombophlebitis
Thrombophlebitis, sometimes called Deep Venous Thrombosis (DVT), can occur after any operation. It is more likely to occur following surgery on the hip, pelvis, or knee. DVT occurs when the blood in the large veins of the leg forms blood clots within the veins. This may cause the leg to swell and become warm to the touch and painful. If the blood clots in the veins break apart they can travel to the lung. Once in the lung they get lodged in the capillaries of the lung and cut off the blood supply to a portion of the lung. This is called a pulmonary embolism. Pulmonary means “lung”. An embolism is a fragment of something traveling through the vascular system. Most surgeons take preventing DVT very seriously. There are many ways to reduce the risk of DVT, but probably the most effective is getting you moving around as soon as possible!
Some of the commonly used preventive measures include:
- Pressure stockings to keep the blood in the legs moving.
- Medications that thin the blood and prevent blood clots from forming.
Infection
Infection can be a very serious complication following an artificial joint. The chance of getting an infection following total hip replacement is probably around 1 in 100 total hip replacements. Some infections may show up very early – before you leave the hospital. Others may not show up for months, or even years, after the operation.
Also, an infection can spread into the artificial joint from other infected areas. Your surgeon may want to make sure that you take antibiotics when you have dental work, or surgical procedures on your bladder or colon to reduce the risk of spreading germs to your new joint.
Stiffness
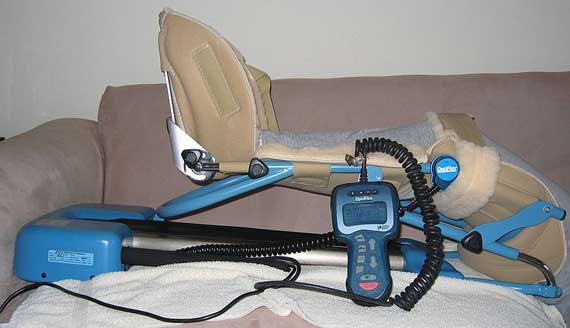
In some cases, the ability to bend the knee does not return to normal after an artificial knee replacement. Many orthopedic surgeons are now using a machine known as a CPM machine (Constant Passive Motion) immediately after surgery to try and increase the range of motion following artificial knee replacement. Other orthopedic surgeons rely on physical therapy beginning immediately after the surgery to regain the motion. It is not clear which is the best approach. Both approaches have benefits and risks, and the choice is usually made by the surgeon based on his experience and preferences.
To be able to use the leg effectively to rise from a chair, the knee must bend at least to 90 degrees. A desirable range of motion should be greater than 110 degrees. Balancing of the ligaments and soft tissues (during surgery) is the most important determining factor in regaining an adequate range of motion following knee replacement, but sometimes increasing scarring after surgery can lead to an increasingly stiff knee. If this occurs, your surgeon may recommend taking you back to the operating room, placing you under anesthesia once again, and forcefully manipulating the knee to regain motion. Basically, this allows the surgeon to breakup and stretch the scar tissue without you feeling it. The goal is to increase the motion in the knee without injuring the joint
Loosening
The major reason that artificial joints eventually fail continues to be loosening of the joint where the metal or cement meets the bone. There have been great advances in extending the life of an artificial joint. Still, most joints will eventually loosen and require a revision. Hopefully, you can expect 12-15 years of service from your artificial knee. In some cases the knee will loosen earlier than that. Just like your diseased knee, a loose joint causes pain. Once the pain becomes unbearable, another operation will probably be required to replace the knee.