Considered one of the most expensive diseases known to man, diabetes can cause damage to virtually all of a person’s organ systems over time. As the condition wears on, it can give rise to a host of new complications, including nerve damage otherwise called diabetic neuropathy.
The symptoms of nerve damage are most pronounced in the distal parts of the body. That’s because these are the areas farthest from the heart, which means blood flow to these parts can be limited and inefficient. The complex interactions between nerves and blood vessels are often damaged in the feet. So they might feel completely numb, or they might feel excruciatingly painful.
In this article, we’re going to dive into the what’s, why’s and how’s of diabetic nerve pain in the feet. Find out what causes it, how to prevent it, and what you can do to effectively treat it and manage the pain.
The Causes of Diabetic Nerve Pain in Feet
Peripheral neuropathy – or damage to any nerves that branch out from the central nervous system – is common in late-stage diabetes. There are a lot of factors that come into play with the development of neuropathy, but much of it starts in the kidney.
To better understand how the nerves in the feet become damaged in diabetes, it’s important to know how they interact with other structures and substances in your body. One of the most important factors that affect nervous health in late-stage diabetes is vasopressin.
This hormone is secreted by the kidney and works to regulate a person’s blood pressure. Alterations in the normal physiology of the kidney can lead to a decreased production of vasopressin, and thus inefficient blood vessel functioning.
This could lead to disastrous complications in the lower limbs when you consider a unique and often overlooked factor – gravity. Ascending blood flow from the lower extremities faces the pull of gravity, which requires the assistance of specialized one-way valves to help push blood back to the heart.
As our muscles push deoxygenated blood from the legs back towards the heart, valves seal off the length of the vessels that have already been travelled. This prevents blood from flowing back to the feet.
When there is a decrease in vasopressin, these one-way valves might not seal. The result is the pooling of blood in the legs and feet, which also explains edema associated with diabetes.
With a lifespan of only 125 days, red blood cells that fail to return to the heart from the lower extremities are left to die and collect in the feet and lower legs. It’s this pooling of waste material that leads to damage in the different tissues in the extremities, including a person’s nerves.
When peripheral neuropathy occurs, signals sent from your receptors to your brain may be impaired. So while your body might be feeling one thing, your brain might interpret it to be something completely different. For instance, a blanket falling over your feet might feel like searing, stabbing, tingling pain.
According to statistics, an estimated 26% of diabetics struggle with some form of chronic neuropathy. And although it might seem like a painful dead end, there are things you can do to help manage the problem.
Can You Prevent Diabetic Neuropathy?
Theoretically speaking, there is no way to prevent diabetic neuropathy. A diagnosis of diabetes means that a specific chain of bodily events has been set into motion. Although stopping these changes in their tracks might not be a feasible reality, there are certain steps you can take to slow down the pace of your developing condition.
In the case of neuropathy, the ultimate and only solution would be to manage your blood glucose levels. By maintaining your blood glucose within as normal limits as possible, you can keep your kidneys functioning properly for much longer. This in turn prevents the decrease of vasopressin, which then maintains proper blood circulation throughout the lower extremities.
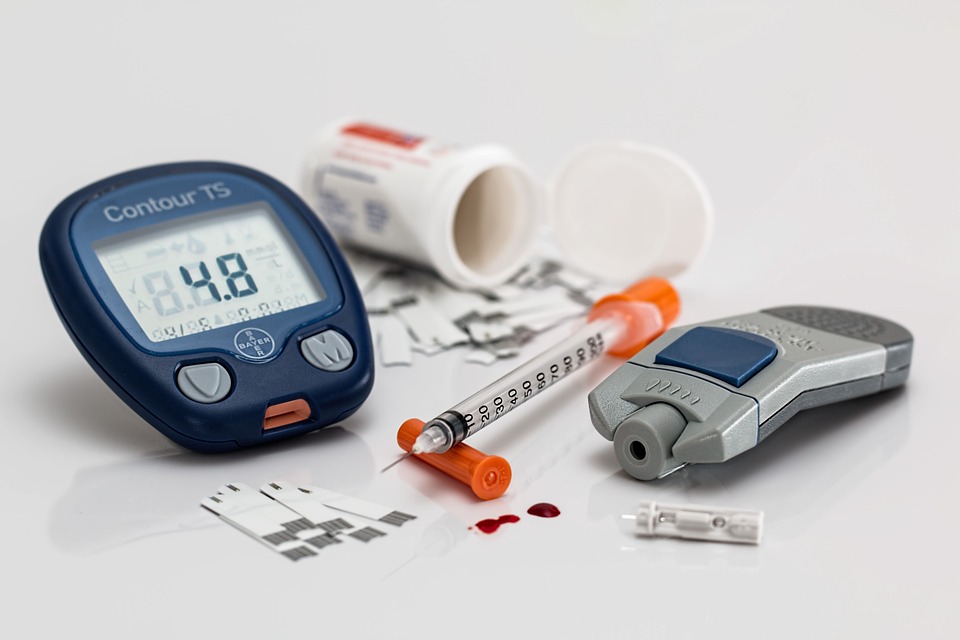
Keep in mind though that the development of neuropathy isn’t a matter of if but of when. That said, you should be aware of the different methods you can put into action to help manage pain and discomfort as they arise.
How to Manage Pain Secondary to Diabetic Neuropathy
Because neuropathy is an irreversible complication, doctors recommend that individuals with diabetic neuropathy do what they can to slow down the progression of nerve damage. This, in combination with pain management techniques, should help you maintain independence and functionality.
Exercise
Even without neuropathy, individuals with diabetes are encouraged to exercise regularly to keep blood glucose levels within normal limits. Maintaining glucose at lower levels will help delay a lot of the complications associated with diabetes, particularly nerve damage.
But other than that, exercise has also been known to increase blood flow. By engaging your lower extremities in physical activity, you can supply affected nervous tissues with nutrient-rich blood. The movement may also assist with ascending blood flow to bring deoxygenated back to the heart.

Recommended exercises for individuals with diabetes are mostly aerobic. These are activities that increase the respiratory and heart rate to help bump up the amount of oxygen that makes it to the muscles. This also helps use up excess glucose so it doesn’t remain stagnant in the system.
Brisk walking, biking, swimming, jogging, and even the simple task of climbing stairs are all suggested aerobic exercises for diabetics. Try to engage in these activities at least thirty minutes a day to help manage neuropathy.
Proper Footwear
There is a multi-million dollar market for shoes and socks specially designed for individuals with diabetes. These products are developed to promote better circulation and provide better comfort and support compared to typical shoe designs.
Some features you’d want to look for include lightweight and breathable construction, antibacterial lining, adjustable design that uses laces or Velcro to optimize fit, and a pliable footbed that accommodates the arches of your feet.
When it comes to diabetic socks, those that don’t dig into the skin will help prevent the obstruction of blood flow. There are also compression socks that snugly fit around your feet and legs to help circulate blood and reduce edema.
Majority of the socks you’ll find will be non-binding. That is, they won’t have seams or thickened elastic bands that could potentially dig into the skin and prevent the proper flow of blood.
Experts suggest that individuals with diabetic neuropathy wear diabetic socks only during waking hours, especially when you expect to stand or walk around a lot. During sleep, diabetics can remove the socks in favor of positional adjustments such as elevating the feet above the level of the chest.
Over-the-Counter Pain Medication
Before you take any sort of pain medication, it’s recommended that you first discuss this management option with your specialist. As they likely have a better understanding of your specific case, they should be able to provide sound advice and suggestions regarding the use of OTC pain meds.
In most cases however, doctors will allow diabetics to take pain medications such as acetaminophen, aspirin, ibuprofen, or naproxen. However, studies have shown that these particular pharmaceuticals are only effective during the early stages of diabetic neuropathy. For advanced cases of nerve damage, the pain might be too pronounced for these OTC medications to resolve.
It’s also worth mentioning that taking such medications as a long-term solution to pain could result to disastrous complications in your liver and kidney. Keep in mind that in diabetics, both these organs are impaired. So pumping them with more synthetic substances to process over a long period of time might result to faster degeneration.
Warm Bath
Soaking in a warm bath may help resolve neuropathic pain, according to numerous studies. Warmth is a modality used commonly in different therapies as a way to improve blood circulation. So soaking your feet in warm water during episodes of pain may help relieve some of the discomfort.
Rolling bubble baths are also highly recommended as the gentle sensations may be soothing and relaxing on the overall. However, it’s important to keep in mind that because of the heightened sense of pain, the initial soak might cause some overstimulation.
When leveraging a bubble bath, be sure to take it slow and avoid rushing through the process. Allow your feet to acclimate to the sensation and soak for only a maximum of 10 minutes at a time. Avoid submerging your feet too long, even if there’s significant pain relief. Skin that’s become soft and moist due to overexposure to water can be easily cut and wounded.
Capsaicin Cream
Capsaicin is the active ingredient found in hot peppers. And while it might cause that burning, stinging sensation when eaten, research has shown that it can help reduce tingling, burning pain.
Over the counter capsaicin cream in concentrations of about 0.1% can be effective to start. So for earlier cases of diabetic neuropathy, this formula can reduce the intensity of mild to moderate pain by up to 11%. As neuropathy worsens however, such small doses may no longer be effective.
Your doctor may be able to prescribe you more potent capsaicin patches with concentrations of up to 8%. However, keep in mind that most professionals will not as easily prescribe these patches as they do come with their fair share of side effects. Only when the benefits outweigh the downsides will your doctor approve their use.
Conclusion
Diabetic nerve pain in the feet is complex, yet it gives us an idea of how our condition might be progressing. By keeping an eye on this complication, you will be better equipped to deal with the disease causing it, allowing you to gauge how far along it has developed.
While the pain might seem inconvenient and hopeless, remember that there are lots of things you can do to help manage it. The most important investment you can make however starts with your overall health.
So when you’re first served that diabetes diagnosis, don’t take it lightly. Take care of your body, watch your diet, and avoid anything that could exacerbate the problem to ensure a happy, healthy life for many years to come.