Your first prenatal exam is very important because it confirms your pregnancy and sets a baseline for comparing your current state of health to your health and your baby’s health as you go through pregnancy. Your first exam includes a physical exam and a gynecological exam which will find out if you are at risk for problems during your pregnancy so these risks can be treated or monitored (watched) to help prevent or lessen complications for you and your baby. High risk conditions include high blood pressure, obesity, severe varicose veins, uterine size, pelvic size and diabetes.
How to Calculate Your Due Date
Your doctor (ob/gyn) will also calculate your due date. To calculate your due date, you need to know the date of the first day or your last menstrual period. Add 7 days to the first day of your last period, subtract 3 months and add one year. Example: Assume the first day of your last period is July 15, 2012 (7/15/2012), then subtract 3 months from 7 months, add 7 days to 15, then add one year to 2012. Your due date is April 22, 2013 (4/22/2013).
Female Reproductive System
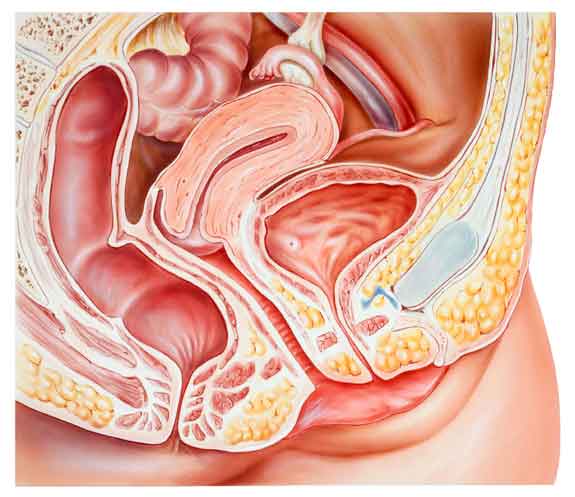
What to Expect During Your First Prenatal Check-up
| Procedure | Purpose |
|---|---|
| Vital signs | Taking your vital signs gives your doctor a baseline for comparing your later prenatal visits. Blood pressure usually goes down slightly during the 1st and 2nd trimesters and then goes back to normal or slightly above normal during the 3rd trimester. |
| TemperaturePulseRespirationBlood pressureWeight | If your blood pressure is above normal during pregnancy and you have other signs and symptoms, it may indicate problems such as pregnancy induced hypertension or preeclampsia.Your baseline weight is used to compare future weight measurements at later prenatal visits. Gaining weight or losing more weight than expected can help assess your nutrition during pregnancy and how your baby is growing developing. A sudden unexplained weight gain can be a sign of preeclampsia. |
| Physical examination | Your first physical exam gives a baseline (starting point) for your overall health status and make sure that you’re starting off your pregnancy in the best physical condition possible. During the physical exam your doctor will check your eyes, ears, nose and throat, chest, lungs, heart, breasts, abdomen, reproductive organs, rectum, and your arms and legs. Special attention will be paid to your breast, abdomen, and pelvic exams as these will change the most during pregnancy. Also, any problems in your breast, abdomen and pelvis may affect childbirth and carrying your baby to full term. |
| Breast examination | Your breasts are checked for lumps, swelling, dimpling, puckering and changes in the texture of the skin texture. This exam provides a baseline for changes that happen to your breasts during pregnancy and for breastfeeding when your baby is born. |
| Abdominal examination | Your abdomen is checked for masses or lumps other than your baby. It’s looked at for scars and stretch marks. You will have an initial measurement of the height of the fundus (the top of your uterus) to give a baseline for future fundal height measurements. Fundul height is measured from the top of the pubic bone to the top of the uterus (the end near your belly button). |
| Pelvic examination | Your pelvic exam confirms your pregnancy and how long you’ve been pregnant. To estimate gestational age: the uterus is the size of an egg at 7 weeks, the size of an orange at 10 weeks and the size of a grapefruit at 12 weeks. You’ll be checked for any pelvic abnormalities that may cause problems during pregnancy or childbirth. The pelvic exam usually includes checking the genitalia on the outside, an examination of the vagina and cervix with a speculum, a Pap smear, a specimen is taken to test for chlamydia and gonorrhea. If you have signs of infection of vaginal specimen will be taken. You will also have a bimanual exam where your doctor will insert one or two gloved and lubricated fingers into your vagina while gently pressing on your lower abdomen with the other hand. This is a to check for:
|
| Recto vaginal examination | This exam will check for the strength and irregularity of the vaginal wall and cervix. The anus is checked for hemorrhoids and fissures and the rectum checked for hernias and masses.Your health care provider puts a gloved finger into your rectum to check the muscles between your vagina and your anus. This also checks to see if there are tumors behind the uterus, on the lower wall of the vagina, or in the rectum. Some doctors put another finger in the vagina, too. This lets the doctor examine the perineal tissue more thoroughly.You may feel like you need to have a bowel movement during this part of the exam. This is normal and only lasts a few seconds. |
| Pelvic measurements | These measurements verify the size and shape of the pelvis to make sure that your baby can pass safely through the birth canal in a normal vaginal birth; if not a cesarean section will be needed. Your doctor may wait until later in your pregnancy to take these measurements when you’re perineal muscles are more relaxed and there is less discomfort while taking the measurements. |
After you’ve had the physical exam, your doctor or midwife will talk to you about what they find and any recommendations they have for you about weight gain, sleep, working while pregnant, intimate relations, smoking, alcohol and drugs. You may also be given a handbook on what to expect during pregnancy.
Lab Tests
Your doctor may order lab tests. These can include:
- Urinalysis to verify pregnancy and to check for urinary tract infection.
- Pap smear
- STD Swabs for chlamydia or gonorrhea
- Yeast infection from trichomoniasis and candidiasis
- Complete blood count
- Hemoglobin and Hematocrit
- Rh factor and Blood type
- HIV test
Return Prenatal Visits
Seeing your doctor or midwife during the rest of your pregnancy is important to assess your needs and the needs of your baby and to see if you are having problems and if you are, then to treat or watch them. If you do not have any complications, then the following is a common schedule for prenatal care visits:
- Every 4 weeks for the first 28 weeks (6 months)
- Every 2 weeks until 36 weeks (6-8 months)
- Weekly until your baby is born (8-9 months)
While you are pregnant, do not take any medicines or drugs without talking with your doctor first. Certain medicines cross the placenta and get to your baby and could be harmful. Avoid alcohol, cigarettes, street drugs such as cocaine, crack, and marijuana, caffeine, and hazardous chemicals.
These medicines are usually safe to take when you’re pregnant, but check with your doctor before taking any over-the-counter medicines. Take your prenatal vitamins every day and always wear your seatbelt.
| Symptom | Medicine |
|---|---|
| Indigestion | Tums, Riopan, Maalox |
| Sinus congestion | Ask your doctor |
| Headache | Regular strength Tylenol |
| Constipation | Metamucil, docusate sodium |
| Dry cough or cold | Robitussin DM |
| Nausea, fatigue | vitamin B6 50 mgs 2 times a day |
Warning Signs During Pregnancy
These are signs or symptoms you should watch for during your pregnancy. These may be signs of a problem and you should let your doctor know if you have any of these.
Signs of Infection
- fever
- vaginal discharge
- painful to urinate
- increased frequency of urination
- marked decrease in urinary output
Signs of Spontaneous Abortion
- vaginal bleeding
- persistent low back pain
- abdominal pain and cramping
Signs of Preeclampsia
- severe, persistent headache
- dizziness
- blurred vision
- sudden swelling of hands, feet, or face
- sudden rapid weight gain
- abdominal pain
Signs of Placental or Fetal Problems
- vaginal spotting or bleeding
- abdominal pain and cramping
- back pain
- noticeable decrease in fetal activity
- no fetal movement
Signs of Preterm Labor (Preterm Birth)
- regular or frequent contractions more than 4 to 6 per hour
- recurring low, dull backache
- menstrual like cramping
- unusual pressure in the pelvis, low back, abdomen, or thighs
When to call your doctor: First trimester warning signs
In summary, if you have any of the following symptoms or warning signs in your first trimester, you should report to your doctor:
- Bright red bleeding
- Dizziness, spots before eyes, or blurred vision
- Gush or leaking water from vagina, vaginal discharge that becomes bloody, watery or significantly increases in amount
- Severe headache unrelieved by rest or Tylenol
- Swelling of hands, feet or face (may be signs of preeclampsia)
- Temperature greater than 100.5 F
- Sharp or constant pain in any part of the body
- Decreased fetal movement
- Uterine contractions or tightening — more than 4 per hour (if earlier than your 37th week, with or without pain)
- Pelvic pressure and menstrual-like cramps
- Low backache that comes and goes
- Intestinal cramps without diarrhea
- An overall feeling that something isn’t right with you or your baby

Things to Avoid in Pregnancy
Foods to avoid in pregnancy
- High mercury containing fish (tuna, shark, king mackerel and swordfish)
- Raw fish or shellfish
- Raw or undercooked meat
- Processed meat
- Raw eggs
- Organ meat (liver, heart, kidney etcetera)
- Caffeine
- Unwashed produce
- Unpasteurized cheeses
Activities to avoid in pregnancy
- Smoking
- Illegal drugs
- Changing the kitty litter box
- Hot tubs
- Extreme sports
- Activities that could cause trauma or force to the abdomen