What Gestational Hypertension & How It’s Treated
If you get PIH, it is very likely that you will have a healthy baby and fully-recover from the disease. This article is for women who may get or already have gestational hypertension (pregnancy-induced hypertension (PIH)), sometimes called Preeclampsia or Toxemia. This disease affects about 5 to 10% of all pregnant women. If you are one of them, you should learn as much as you can about it so you can help your health care provider keep you and your baby healthy. Pregnancy-Induced Hypertension (PIH) can remain under control with treatment long enough for you to deliver a healthy, mature baby or it can become a serious problem for you and your baby almost without warning. The most important things you can do are:
• know if you are at risk so you can tell your health care provider,
• continue regular pre-natal care,
• follow your health care provider’s instructions for controlling PIH and
• tell your doctor or PIH specialist right away of any symptoms during pregnancy.
If you get PIH, it is very likely that you will have a healthy baby and fully-recover from the disease. But it will take alertness and skill on the part of your health care provider and full cooperation from you. The rewards for you and your baby are well worth it!
What is pregnancy-induced hypertension (PIH) (also called gestational hypertension)?
If you are pregnant and your systolic pressure is 140+ or the diastolic pressure is 90+ on several readings, it is too high.Pregnancy-induced hypertension (PIH) is a type of hypertension (high blood pressure) that happens only during pregnancy. It can be mild or become very serious. The chart under the heading “How will I know if I have PIH?” shows the different stages and symptoms of PIH.
PIH may develop slowly or come on suddenly without warning anytime during your pregnancy, during labor and even just after you have your baby.
There is no cure for PIH while you are pregnant; the only cure is to deliver your baby. But there are treatments and medicines to (1) help you from becoming more ill, (2) to prolong the pregnancy so your baby becomes more mature and (3) to help you and your baby get through delivery safely. After delivery, the disease eventually goes away. You may have to continue taking medicines and seeing your doctor or specialist but you shouldn’t have any lasting effects of the disease.
How common is gestational hypertension (PIH)?
The more serious stage of Pregnancy-Induced Hypertension, called preeclampsia, occurs in 5-10% of all pregnant women. Of women with preeclampsia, only about 5% will get the most serious stage of the disease, called eclampsia.
What happens when you have PIH?
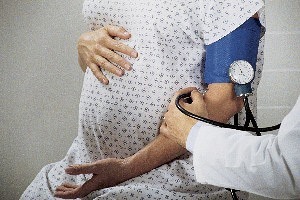 Hypertension means the pressure that your blood exerts against your artery walls as your heart pumps blood through the body is higher than it should be. Higher-than-normal blood pressure is one of many conditions that happens when women get pregnancy-induced hypertension, but is not what causes the disease. PIH starts with vasospasms—like muscle spasms—in the arteries.
Hypertension means the pressure that your blood exerts against your artery walls as your heart pumps blood through the body is higher than it should be. Higher-than-normal blood pressure is one of many conditions that happens when women get pregnancy-induced hypertension, but is not what causes the disease. PIH starts with vasospasms—like muscle spasms—in the arteries.
At the most serious stage of PIH, these vasospasms can cause:
• damage to artery walls
• a build up of blood platelets and other blood products that form blood clots; this build-up causes a narrowing of the space in your arteries, which cuts down the amount of blood and oxygen flowing to organs like the brain, kidneys and liver
• a drop in the amount of platelets, which can cause spontaneous bleeding
• torn cells that break open and dump toxins, which causes more damage to organs and high blood pressure, and which, if left untreated, can cause stroke
• leaky blood vessels that can cause severe swelling of face, eyelids, hands, legs, feet and sometimes the brain (cerebral edema); swelling in the brain can cause seizure, which, in turn, can cause early birth, a lack of oxygen to the baby or a loss of blood supply to the placenta
• serious damage to or even failure of kidneys and liver
Remember – only a small percentage of women with PIH experience the most serious stage of the disease. Telling your health care providers of any risk factors that you have, getting regular pre-natal care and alerting your doctors to any symptoms are critical to the continued good health of you and your baby.
What causes PIH?
The simple answer is doctors and scientists don’t know what causes PIH. Some studies suggest that PIH may be caused by the mother’s poor diet, an “allergy” to the placenta and fetus or even family history. But after many years of research, there is no clear answer to what triggers PIH. There are, however, risk factors for who is more likely to get PIH, as follows:
Risk Factors for Pregnancy Inducted Hypertension
• if this is your first pregnancy
• if you had PIH with an earlier pregnancy
• if you have a family history of PIH
• if you had high blood pressure before you became pregnant
• if you are younger than 20 or older than 34
• if you have lupus, diabetes or kidney disease
• if you were obese before pregnancy
• if you are pregnant with more than one baby
• if you did not have regular pre-natal care and/or a poor diet
• if you have a hydatiform mole
• if you are African-American
• if there is something wrong with your baby (e.g., chromosomal abnormality) or with your placenta (e.g., maternal serum alpha feto protein – MSAFP)
How will I know if I have PIH?
Diagnosing PIH starts with your first pre-natal visit. If you have one or more of the risk factors shown above, then your pre-natal health care team should be on the alert for (1) high blood pressure, which is the first sign, followed by
(2) protein in your urine. This may happen early in your pregnancy or not until the end. Most often, it occurs after the 20th week or so of your pregnancy and lasts until a week after childbirth.
On each pre-natal visit, your health care provider should (1) weigh you, (2) take your blood pressure, and (3) get an early-morning urine sample to check protein levels.
The chart below shows the stages of PIH, the medical problem your health care provider will look for and the symptoms you may have.
| STAGES OF PIH | MEDICAL PROBLEM | YOUR SYMPTOMS |
| Early Pregnancy-Induced Hypertension (PIH) | Systolic blood pressure that is greater than 30mmHg or diastolic blood pressure that is greater than 15mmHg over baseline (your blood pressure at the start of your pregnancy). Also blood pressure greater than 140/90mmHg after 20 weeks gestation. | No obvious symptoms. |
| Preeclampsia | PIH with proteinuria (protein in your urine) or edema (swelling) or both after 20 weeks gestation. | • Sudden weight gain or gaining more than a pound a week especially in the last trimester. • Swollen face, hands and feet which worsens in the morning • Headaches • Blurred vision • Seeing spots • Persistent painful heartburn • Decreased production of urine (oliguria) |
| Severe Preeclampsia | Systolic blood pressure that is greater than 160mmHg or diastolic blood pressure that is greater than 110mmHg, with high levels of protein in your urine, oliguria, and fluid in the lungs or cyanosis. | • Hyperflexia • Nausea or vomiting • Epigastric pain (pain between your sternum and navel) |
| Eclampsia | When preeclampsia is accompanied by seizure. | • Symptoms worsen • Convulsion preceded by hyperflexia (overactive reflexes), muscle twitches •Coma • Nausea or vomiting • Epigastric pain (pain between your sternum and navel) |
| HELLP syndrome (Hemolysis, Elevated Liver enzymes and Low Platelets) | This is a severe form of PIH in which the liver is affected. It is a medical emergency and requires that your baby be delivered. | • Epigastric pain (pain between your sternum and navel) or right upper quadrant tenderness (just under your ribs on your right side) • Nausea or vomiting • Headache • Tired, listless. • Jaundice (yellow skin, eyes) • Hematuria (blood in your urine) |
Important note: In the early stage of PIH, you probably will not have any symptoms, which is why it’s so important to tell your health care providers of any risk factors you have. Later on, if your disease gets more serious, you may feel some of these symptoms or all of them. Don’t worry or try to guess about symptoms. Tell your doctor or specialists whatever you are feeling and let them decide the best way to treat you.
How will I be treated for PIH?
If you are considered high risk for PIH
If you are considered high risk for PIH (for example, you have diabetes or a family history of preeclampsia), your health care provider may:
• Recommend more frequent office visits after 24 weeks of pregnancy. If you develop any warning signs of preeclampsia (weight gain or swelling), tell your doctor right away.
• Have you check your weight and blood pressure at home.
• Prescribe one baby aspirin per day throughout your pregnancy, which may protect you from developing preeclampsia.
• Send you to a perinatologist, an obstetrician who specializes in high-risk pregnancies.
• Remind you that a good diet should include:
Daily Food Guide During Pregnancy
| Food Group | Servings | Choose From (1 serving equals) |
| Protein Foods | 6 | 1 oz. Lean beef, pork, lamb, veal, chicken, fish or cheese¼ cup cottage cheese1 egg1 tbsp. peanut butter |
| Milk Products | 4 | 8 oz. Low fat milk or yogurt |
| Breads & Cereals | 6 | ½ cup cereal½ cup cooked rice or pasta1 slice bread6 crackers |
| Fruits | 5 | ½ cup (4 oz.) fresh fruit or juice¼ cup dried fruits such as raisins or prunes1 whole small apple, pear or orange |
| Vegetables | 5 | ½ cup cooked vegetables such as broccoli, carrots or greens1 cup raw vegetables |
Be sure to follow all dietary advice your doctor gives you. You may be put on a low sodium diet to reduce the amount of salt your eat or the DASH Diet which has been shown to lower blood pressure. You should avoid foods and drinks that contain caffeine like sodas, coffee and chocolate. You may need to restrict your salt intake by eliminating table salt from your meals and avoiding foods high in salt. To find out if a food is high in salt, read the label of any foods before you eat them and look for sodium content. Be sure to take your prenatal vitamins. Learn more about pregnancy weight gain and where the weight goes during pregnancy.
If you get mild preeclampsia and your baby is not in danger
There are several things your health care provider may recommend if you get mild pregnancy-induced hypertension (preeclampsia) and your baby is not in danger.
• Bed Rest – Rest often. Many women can reduce their high blood pressure by resting in bed for a few days. Lying on your left side helps to improve blood flow.
• Add Protein to Your Diet – If the disease is causing you to lose protein in your urine, you may be helped by a high-protein diet to replace the lost protein.
• Check you and your baby – A visiting nurse can check your weight, your blood pressure, your urine for protein and listen to the baby’s heart rate in your own home. You can even be trained to do these things for yourself with a scale, blood pressure monitor, urine test strips and an external fetal heart rate monitor.
• Test your blood – If your health care provider becomes concerned, you may need to have a blood test in the office to check for poor kidney function, abnormal liver function and/or a drop in the amount of platelets in your blood.
• Test you further in the hospital – If your symptoms and test results show that you are developing severe preeclampsia, your health care provider may want to put you in the hospital for more tests for you and the baby, as well as around-the-clock monitoring.
If you get severe preeclampsia
If your mild preeclampsia becomes more serious preeclampsia, you will be hospitalized and prepared to deliver your baby. The goal of your doctors, nurses and other specialists at this time is to stop your condition from getting worse, while making sure your baby is not in distress before it’s time to deliver. Here’s what you can expect in the hospital:
• A doctor or specialist will take your medical history and perform a physical exam.
• Blood tests will be done for the latest findings.
• A fetal monitor will check your baby’s heart rate and you may have an ultrasound for further evaluation of your baby.
• If you are delivering your baby before the due date, you may have an amniocentesis; this is a test that uses a needle to draw amniotic fluid from around the baby to measure if your baby’s lungs are mature.
• You will probably be given medicines to help you and your baby come through labor and delivery in the safest way possible.
Medicines to help you and your baby
Your doctor or other specialists may give you one or more medications during your pregnancy, labor and delivery. If you are given drugs, which type and how much will depend upon (1) the overall health of you and your baby, (2) how far along your disease is and (3) the maturity of your baby just before delivery.
Generally medications are used to:
• Lower blood pressure
• Treat cell damage caused by spasms
• Prevent seizures and convulsions
• Decrease breathing problems in premature babies
• Decrease the risk of brain hemorrhage and intestinal problems in premature babies
Labor and Delivery
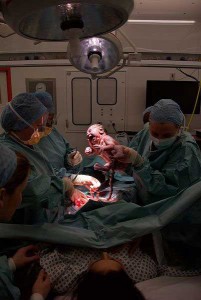
Your doctor, the anesthesiologist and any other specialists who will help with your baby’s birth will decide whether you can deliver your baby vaginally or by cesarean section (c-section) and what kind of pain medicine will work best for you. Normal labor and vaginal delivery are preferred if your cervix is dilated and you and your baby are healthy and strong enough. You should also learn about induced labor. If you or your baby are under any stress because of your disease, your doctor will probably perform a cesarean.
If you develop complications of preeclampsia during labor or delivery (e.g., you are in danger of having a stroke, or show signs of kidney failure), one of your health care team specialists will explain any other treatments that might become necessary. Be assured your health and the health of your baby are their utmost concern.
What will happen after I have my baby?
For the first few days after you deliver your baby, the hospital staff will keep a close watch on you. In all likelihood, your PIH will go away and you will be on your way to a full recovery. However, if your PIH became very serious, your health care providers will closely monitor you. They will check for excess blood loss, any effects of the drugs used during delivery or any damage to your kidneys or liver. If any problems are found, treatment will begin immediately and may continue for a while. If your baby was born prematurely, your baby may have to remain in the hospital for further care.
Don’t Panic!
Don’t panic if you have been diagnosed with pregnancy-inducted hypertension. It is a condition that is treatable. Most mothers and babies come through it fine. But don’t ignore it either.
Call your doctor if you:
• have severe headaches
• have changes in your vision
• gain more than 3 pounds in 24 hours
• have nausea, vomiting, diarrhea, cramping abdominal pains
• have excessive irritability
• have other symptoms that worry you
For the healthiest pregnancy and delivery, remember these things:
• Know if you are at risk and tell your health care provider
• Have regular pre-natal care
• Eat a healthy diet, get plenty of rest (lay on your left side to help circulation) and avoid stress
• Follow all your doctor’s instructions
• Don’t worry or guess about symptoms, tell your health care team
• If you take good care of you, you will be taking good care of your baby
Glossary
• Cesarean Birth: Delivery of a baby and the placenta through an incision made in a woman’s abdomen and uterus.
• Eclampsia: The end stage of pre-eclampsia. Seizures occurring in pregnancy and linked to high blood pressure.
• Placenta: Tissue that provides nourishment to and takes away waste from the fetus.
• Preeclampsia: A condition of pregnancy in which there is high blood pressure, and protein is present in the urine and ranges from mild to severe.
• Prenatal Care: A program of care for a pregnant woman before the birth of her baby.