Gallbladder Anatomy
 The gallbladder is a small pear-shaped, gray-blue*, sac-like organ located on the under-surface of the right lobe of the liver in the upper right quadrant of the abdomen. Ducts (tubes) connect the gallbladder to the small intestine (duodenum). The gallbladder is divided into the fundus, body and neck. The liver makes 3-5 cups of bile every day. The main function of the gallbladder is to collect and store the digestive juice called bile that is secreted by the liver. The bile is then passed through cystic ducts into the bile ducts and finally into the intestine to aid in the digestion process when food is eaten, especially fatty foods. When the gallbladder is taken out, this function is taken over by the liver and its ducts. Problems with the gallbladder interrupt the total functioning of the digestive system. (*shown as green in the image)
The gallbladder is a small pear-shaped, gray-blue*, sac-like organ located on the under-surface of the right lobe of the liver in the upper right quadrant of the abdomen. Ducts (tubes) connect the gallbladder to the small intestine (duodenum). The gallbladder is divided into the fundus, body and neck. The liver makes 3-5 cups of bile every day. The main function of the gallbladder is to collect and store the digestive juice called bile that is secreted by the liver. The bile is then passed through cystic ducts into the bile ducts and finally into the intestine to aid in the digestion process when food is eaten, especially fatty foods. When the gallbladder is taken out, this function is taken over by the liver and its ducts. Problems with the gallbladder interrupt the total functioning of the digestive system. (*shown as green in the image)
Gallbladder problems include:
• cholelithiasis (gallstones), where solid components of the bile from stones of various sizes. Gallstones can get in the bile duct, blocking the flow of bile causing swelling of the gallbladder and pain in the abdominal area. Cholelithiasis is associated with abdominal pain in the right upper quadrant all the way up to the right shoulder and may occur after fatty meal. Symptoms of jaundice may also go with cholelithiasis. Gallstones are found in about 15% of men and 30% of women in the U.S.
• cholecystitis, which is the inflammation of the gallbladder due to infections. The most common symptoms of cholecystitis is sharp abdominal pain on the right side along with nausea, bloating, fever, vomiting and jaundice if gallstones are in the common bile duct. Cholecystitis can happen suddenly (acute) or over a longer period (chronic).
• perforated gallbladder is a condition where the gallbladder leaks or bursts. This happens rarely, but it can be life threatening.
Gallstones are usually diagnosed by ultrasound—a safe, painless, and non-invasive technique that uses high frequency sound waves to create an image of the gallbladder and gallstones. In order to relieve symptoms and complications, the gallbladder is removed surgically, called cholecystectomy.
Cholecystectomy Procedure
Cholecystectomy is the surgical removal of the gallbladder. More than 500,000 procedures are performed each year in the U.S. Cholecystectomy is usually done for gallstones and can be performed in two ways:
• open cholecystectomy
• laparoscopic cholecystectomy
Risks, Benefits, and Complications of Cholecystectomy
The benefit of having your gallbladder removed is relief of pain and most likely stop gallstones from coming back. If you don’t have gallbladder surgery, you risk the possibility of your symptoms getting worse, infection or the gallbladder bursting and infecting your abdominal cavity. Although there is some risk with all surgery, gallbladder removal is a very common surgery and the risks are small. Possible complications involved in open cholecystectomy are:
• bleeding
• injury to the common bile duct
• numbness
• raised scars
• hernia at the incision site
• puncture of the intestine
• wound infection
• abscess formation
• respiratory problems (pneumonia)
• deep vein thrombosis (blood clots)
Risks are lower with laparoscopic cholecystectomy. However, while inserting instruments and performing surgery, there is risk of injury to the common bile duct, which is the connection between the liver and the gallbladder. Minor injuries to the common bile duct are treated non-surgically, but major injuries can cause severe infection and pain and need corrective surgery.
Preparing for Cholecystectomy
Like any other surgical procedure, you will have to sign an informed consent that says you understand the procedure, its risks and potential complications and agree to have the surgery.
You shouldn’t have anything to eat or drink after midnight before the day of surgery. You can usually take your daily medicines on the morning of surgery with a sip of water. Talk to your surgeon before taking blood thinners that morning. If you smoke, quit smoking and using tobacco products before surgery and while you are healing; nicotine has been shown to slow down the healing process. Do not use nicotine patches or gum as they also put nicotine into your system.
Anesthesia
Both surgical techniques are done under general anesthesia by a general surgeon. You will meet with the anesthesiologist before your operation. Be sure to let them know any problems you have had in the past with anesthesia or surgery. Also let them know if you:
• have any allergies
• have loose teeth or dental work
• have heart or lung disease
• have any health condition including stomach problems
• smoke, use alcohol or drugs
• take vitamins or supplements
• take daily medicines and what those are
With general anesthesia you will be asleep during the surgery and will not feel any pain.
What to Bring to the Hospital
• Insurance card and picture identification (driver’s license)
• Advance Directives
• Your glasses or dentures
• Loose fitting, comfortable clothes
• List of any medicines you take every day
Do not bring anything of value to the hospital such as jewelry, money, or electronics. The hospital will not be responsible if they are lost or stolen.
Prior to Cholecystectomy
You will get an ID bracelet on admission and taken to a presurgery area to change into a gown and have an IV placed in your arm or hand. The IV will be used to give you medicines and fluids. You may receive medicine to help you relax before they take you to surgery.
Open Cholecystectomy
This is the older procedure involving a 4 to 6 inch up-and-down incision in the right upper portion of the abdomen, or a slant incision just below the ribs on the right side. The peritoneum is cut and the gallbladder is removed. The incisions are then closed. In order to prevent accumulation of fluid at the incision site, drains may be used. The drain is usually removed in the hospital. The procedure takes about 1-2 hours. If there are no complications following surgery, you will be in the hospital for one to three days followed by 4 weeks’ rest at home before you can get back to your normal lifestyle. In more complicated cases, it may be 4 to 8 weeks before you get back to normal activity.
Laparoscopic Cholecystectomy
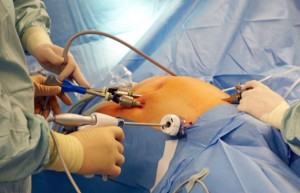
Laparoscopic cholecystectomy, often called “lap choly” is the latest procedure and is extensively used worldwide. During laparoscopic cholecystectomy, the surgeon makes four very small incisions (slits) of less than half an inch each. One slit is at the belly button, two are on the right side below the ribcage, and one is in the upper portion below the sternum, or breastbone. A tube is inserted into one of the slits and the abdominal cavity has been filled with carbon dioxide gas to inflate the area so the surgeon can see to work inside. A laparoscope is inserted in one of the other slits. A laparoscope is long tube with a small video camera and light on the end. This camera is connected to a video monitor, where the surgeon gets a good view of the organs and can do the surgery accurately. The other incisions are used to insert various instruments to grasp and remove the gallbladder. The surgeon guides the laparoscope while watching the view it provides on a video monitor. The gallbladder is separated from the common bile duct and removed with a grasper tool through one of the incisions. Once the gallbladder is removed, the carbon dioxide gas is removed and all incisions are sutured or closed with tape strips. The procedure takes 1-2 hours.
In about 1 in 30 to 40 cases, the surgeon may start with laparoscopic surgery, but complications may cause the technique to be changed to open surgery. Complications include a severely diseased gallbladder, not being able to see the organs clearly, or the instruments cannot be used without risks. It’s important to know that even though you are expecting to have a laparoscopy, there is a chance of having an open cholecystectomy.
The need to convert from laparoscopic to open surgery is more common if:
• you are over age 65
• male
• have a history of acute cholecystitis
• have had prior abdominal surgery
• have a high fever or high bilirubin
• repeated gallbladder attacks
• other diseases that limit your activity
After Cholecystectomy
You will be taken to the recovery room until you wake up and are past any problems from the surgery. Careful attention is given in recovery as with any major surgery. Your blood pressure is monitored closely as well as your pulse, breathing and temperature.
Moving and deep breathing will help prevent fluid in your lungs and pneumonia. An effective way to breath deeply is to take a deep breath and hold it for 5 seconds. Take 5 to 10 deep breaths every hour while you are awake. Because of the anesthesia and not moving around, your risk of getting blood clots in your legs is increased. During surgery you may have had sequential compression stockings to help prevent blood clots. After surgery, it is important to get up as soon as possible and walk around to prevent blood clots.
It’s normal to feel tired for several days and you may need more sleep than usual. Don’t drive until your pain is under control without narcotics and your surgeon says it’s OK.
After Open Cholecystectomy
You may not be able to breathe deeply due to the effects of anesthesia or because of pain. Pain medications will be given to relieve pain. Be sure to let the nurses know if the pain medicine is not working. Controlling pain is very important; you want to feel like moving around and taking deep breaths, which will help prevent complications that can make your recovery take longer. Doing deep breathing exercises is very important in preventing pneumonia. The nurses will show you how to support to the incision with a pillow (splinting) while doing deep breathing exercises or coughing. Your incision site is checked for drainage and infection.
Your diet will start as intravenous fluid and then slowly you will be given a regular diet as your bowel activity returns to normal and any nausea has stopped. It’s normal to have loose bowel movements for a few days after surgery. Pain medicine can cause constipation. If you are constipated increase the fiber in your diet or try a stool softener. Foods high in fiber include grains, fruits and beans.
You will go home in about 3-5 days. Slowly increase your activities. Do not lift of do any strenuous activity for 3-5 days. Returning to normal activities takes four to six weeks after surgery depending on your overall health and whether you had any complications.
Wound Care. Do not soak in a bathtub until your stitches or staples are removed and your wound has healed. It’s OK to take a shower unless your surgeon tells you not to. Protect the new skin of your incision from the sun as it can cause darker scarring; keep it out of the sun or wear sun screen for at least a year. Wear clothes that don’t rub against your incision. Change your bandages just as your surgeon prescribes and always wash your hands before and after touching near your incision site. Your scar will heal in about 4 to 6 weeks; it will get softer and fade over the next year. The feeling around your incision will come back in a few weeks or months.
After Laparoscopic Cholecystectomy
Pain from surgery can probably be controlled with pills. The abdominal pain can be accompanied with nausea and/or vomiting. Let the nurses know if you are nauseated; they can give you medicine to relieve the nausea. Liquids are OK to drink within 6 to 8 hours of surgery; solid food is allowed the day after the surgery. Pain medicine can cause constipation. If you are constipated increase the fiber in your diet or try a stool softener. Foods high in fiber include grains, fruits and beans.
Discharge from hospital is generally the same day. Slowly increase your activities. Do not lift of do any strenuous activity for 3-5 days. Returning to normal activities takes around 7 to 10 days. However, if you have other health conditions, you may have a longer hospital stay or recovery at home and a longer recovery period.
Wound Care.
Do not soak in a bathtub until your steri-strips fall off (7-10 days) and your wound has healed. It’s OK to take a shower unless your surgeon tells you not to.
Biopsy
After the procedure, the gallbladder is sent for biopsy to confirm the diagnosis of either cholelithiasis or cholecystitis. The biopsy also helps to find cancer. If cancer is found, the patient might need to undergo another surgery to remove part of the liver or lymph nodes that are affected.
When to Call Your Surgeon
When you are discharged the nurses will tell you when to make an appointment for follow-up with your surgeon. Stitches or staples will be removed at follow-up. If you think you have a fever, take your temperature. If you have any of the following, you should contact your surgeon right away:
• Pain that gets worse or will not go away with your pain medicine
• A fever of more than 100.5°F
• Vomiting
• Strong abdominal pain
• No bowel movement or cannot pass gas for 3 days
• Watery diarrhea that lasts longer than 3 days
• If you have drainage from your incision
• If the edges of your incision separate
If you have symptoms of a life threatening emergency call 911.
Prognosis
A small number of people are affected with post cholecystectomy syndrome, which has symptoms like gastrointestinal distress and/or constant pain in the right upper quadrant of the abdomen. Some others can develop chronic diarrhea after surgery. This can happen since the surgery causes disturbances in the bile duct. Most of the time no treatment is needed and clears up on its own within a few weeks. Many people have no symptoms at all after having their gallbladder removed.