Cumulative trauma disorders (CTDs) are injuries of the musculoskeletal system—including the joints, muscles, tendons, ligaments, nerves, and blood vessels that are often grouped together as CTDs, Repetitive Stress Injury (RSI), overuse syndrome, and repetitive motion disorders. CTDs are the largest work-related health problem in the U.S. CTD symptoms develop from the accumulation of repeated small injuries or stresses to our musculoskeletal system. CTD is not disease but a response to excessive or repeated demands on our body without enough time to recover before adding more stress. This article explains some of the concepts of CTD, what can cause CTD and how CTD causes symptoms. There are links to articles on our site many common CTDs as well as links to anatomy and function articles for the subject injuries.
- Cumulative: Repeated small injuries add up to a larger injury or syndrome
- Trauma: An injury to the body from a physical cause.
- Disorder: A problem with normal body functions. Syndromes are a group of signs or symptoms—like pain, tingling or weakness—that are linked by a common anatomical history.
Causes of Cumulative Trauma Disorders
CTDs are usually caused by a combination of risk factors:
- repetitive motions, that is making the same motion over and over like hammering a nail
- motions using force like pulling, pushing, lifting, and gripping
- awkward posture or body positions that are unnatural resting positions
- holding the same body position without moving or resting for long periods
- mechanical compression of soft tissues in the hand against hard edges or ridges: like tools or objects that press against the palm
- fast movement of body parts like swinging your arms
- vibration, especially in cold conditions, like using vibrating hand tools
- mental stress can cause muscles to tighten and restrict blood flow
- not enough recovery time with overuse like rest breaks or days off. This also increases other CTD risk factors.
CTDs which usually affect the arm and hands:
- carpal tunnel syndrome
- wrist tendonitis
- ulnar nerve entrapment
- epicondylitis (elbow)
- shoulder tendonitis
- hand-arm vibration syndrome
Common symptoms of CTDs include pain and swelling of the affected body part. Although back injuries are not considered CTDs, they often result from similar risk factors as CTDs. Some work and play activities have more risk factors than others. However, it’s possible to reduce your risks and prevent CTDs. We’ve said overuse can cause problems, but what’s really happening? Muscle Tension + Repetitive Motion + Over Use + Incorrect or Static Posture = CTD
Muscle Tension
To work properly, the body and its parts need a steady blood supply, rich in oxygen and nutrients. Cutting off or reducing the blood supply injures body tissues. When muscles are tense, they squeeze off the blood supply which is their source of energy and fuel. Muscles can get energy without oxygen however, the process produces lactic acid, a potent pain causing chemical. As the pain gets worse, the muscles keep tightening to protect the injured area—slowing down the blood supply even further. When nerves don’t have enough blood plus the area is being squeezed by tense muscles, the nerves begin to tingle (that pins and needles feeling) or even go numb.
Repetitive Motion
Repetitive motion injuries cause tissue damage from repeated trauma—like writing, painting or typing. Almost any activity that produces repeated small trauma to an area of soft tissue—tendons, nerves, muscles—can lead to CTD. Trauma happens when muscles and joints perform the same movement over-and-over.
Over Use
Using muscles and joints after they’re tired increases the chances of injury. When muscles or tendons are overloaded or overworked they don’t get enough rest and don’t have a chance to fully recover.
Incorrect or Static Posture
Incorrect standing and sitting postures put abnormal stress on the body causing pain and stiffness. Our joints are made to move—even correct posture held for too long is considered overuse.
Types of Cumulative Trauma Disorders
CTDs are basically disorders of tendons—which are part of the muscles—or nerves.
Tendon Disorders
Tendons are fibrous tissue that connect muscles to bones. Tendon disorders and their protective coverings, called synovial sheaths, are the most common CTDs. CTD symptoms include:
- a dull ache over the inured tendon
- tenderness when touched
- discomfort with certain movements
- disabling pain with repeated injury without treatment
Common tendon CTDs:
- Tendonitis is inflammation in the tendon caused when a muscle/tendon is used repeatedly. With normal use, the small fibers that make up tendons get small tears our body can easily repair. With continued overuse and without enough time to recover, the tears aren’t able to completely heal. Tendons of the wrists, elbows and shoulders are most often affected. Risk factors at work or play that cause tendonitis include:
- repetition
- force
- awkward or static posture
- over-extension (excessive stretching) of muscles
- fast movements
- vibration
Without enough rest to allow injured tissues to heal permanent damage can result.
- Tenosynovitis is a general term for irritation of the tendon’s synovial sheath caused by unnatural positions, force or pressure, along with other CTD risk factors. Irritation stimulates the sheath to produce too much synovial fluid. The fluid accumulates causing the sheath to swell and be painful. Other symptoms include tenderness, cracking sounds, and often the loss of some function in the affected body part. A poorly arranged work station, poorly designed tools, and even bad work habits are causes tenosynovitis.
- Stenosing tenosynovitis is a form of tenosynovitis. Tightening of the tendon’s synovial sheath is caused when the surface of the tendon gets irritated, rough, and swollen. Repetitive motions that put stress on the tendons, such as twisting of the hand and forceful gripping, cause abnormal thickening of the sheath and constriction of the tendons.
- de Quervain’s tenosynovitis is from chronic friction between the two tendons in the thumb and the sheath they share. de Quervain’s is the most recognized type of stenosing tenosynovitis. The thumb motion is restricted by the swollen tendons. Jobs with a high rate of de Quervain’s include buffers/grinders, sewers and cutters, packers, and housekeepers.
- Rotator cuff tendonitis, the most common shoulder tendon disorder, is often associated with jobs that require the elbow to be in an overhead position for long periods of time. This position puts stress on the shoulder tendons causing tearing and swelling of the rotator cuff tendons. Repeated overhead motions cause thickening of the tendons and the tissues of the arm sockets. This can lead to “frozen shoulder” syndrome, which may include severe pain and the loss of shoulder function.
- Ganglionic cysts are also a tendon sheath disorder. A bump on the wrist forms under the skin from the sheath swelling up with synovial fluid from repetitive motion, such as prolonged typing or keyboard use.
- Golfer’s elbow (medial epicondylitis) is inflammation of the epicondyle of the humerus in the elbow caused by repeated or forceful rotation of the forearm while bending the wrist at the same time. Epicondylitis is common in construction jobs and assembly work.
- Tennis elbow (lateral epicondylitis) is inflammation of the extensor tendons that attach to the outside of the elbow. It’s caused by rapid over-arm motions like throwing. Athletes aren’t the only ones affected. Most cases are caused by job-related cumulative trauma.
- Trigger finger happens when the tendon sheath of a finger is so swollen that the tendon becomes locked in the sheath. The ring and middle finger are most often affected. Trigger finger is usually caused by using tools with handles that have hard edges or ridges, and/or repetitive forceful gripping. The pain is not usually severe, but moving the finger causes snapping and jerky movements.
- Bursitis is inflammation of the bursae, small flat sacs filled with synovial fluid that prevent friction between tendons and muscles over bony areas like our shoulders, elbows, and knees. A tendon that gets rough from overuse irritates the bursa next to it causing the bursa to swell. Shoulder bursitis can make it hard to move the shoulder and limit movement.
Nerve Disorders
Pressure on the nerves pressing against hard edges or of work surfaces, tools, or nearby bones during repeated activities can result in cumulative trauma disorders of the nerve. The most common type of nerve CTDs:
- Carpal tunnel syndrome (CTS) is an increasingly common CTDs. CTS refers to compression of the median nerve as it passes the carpal tunnel in the wrist. Any condition that increases the contents or decreases the size of the carpal tunnel can compress the median nerve. Jobs that combine high force, high repetition, awkward hand posture and little rest—like typing, assembly work, packing, bricklaying, sewing, and cutting—are at high risk for CTS. Symptoms of CTS include numbness, burning, and tingling in the first 3 ½ digits. If left untreated, symptoms can become much worse and result in the loss of grip strength, clumsiness, increased pain at night, and possibly permanent loss of hand function.
- Raynaud’s syndrome is also referred to as “vibration white finger” or “hand-arm vibration syndrome.” This condition is caused by forceful gripping and/or long-term use of vibrating tools like hand-held power drills, power saws, nail guns, chipping hammers, and rotary hammer drills. Using vibrating tools in cold temperatures increases the risk of Raynaud’s syndrome. Symptoms include numbness and tingling in the fingers, skin that turns pale and cold, and ultimately loss of feeling and muscle control in the fingers and hands.
- Thoracic outlet syndrome (TOS) involves the compression of nerves from the spine and blood vessels from the heart that go to the muscles in the arm. TOS is caused by doing overhead tasks for long periods of time. Symptoms of thoracic outlet syndrome include numbness in the fingers, a weakened wrist pulse and feeling like one’s arm “is asleep.” Thoracic outlet syndrome is often mistaken for being carpal tunnel syndrome.
- Other nerve entrapment syndromes. Repetitive motion of the upper extremities can also entrap the median, ulnar, and radial nerves in other areas. Pronator teres syndrome involves entrapment of median nerve in the forearm. Cubital tunnel syndrome involves entrapment of ulnar nerve from outside pressure over the cubital tunnel at the elbow. Radial tunnel syndrome refers to entrapment of the radial nerve by the extensor muscles of the forearm.
Treatment of Cumulative Trauma Disorders
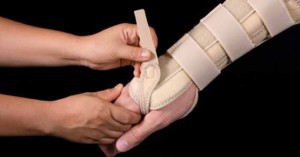 If you’re diagnosed with a CTD, there are many conservative, non-surgical treatments to relieve discomfort from overuse. Splints may be recommended as an early treatment to protect and rest sore areas. Anti-inflammatory medicines are often used along with physical therapy like ice packs, ultrasound, or electrical stimulation. Special exercises help tissues move safely while they heal. Assess both your work and recreational activities to figure out if they are adding to your problem. Keep in mind that tension restricts the flow of blood causing muscles and nerves not to get enough oxygen and nutrients, aggravating the symptoms of CTD. Resting the injured area during work and play can relieve tension and allow recovery.
If you’re diagnosed with a CTD, there are many conservative, non-surgical treatments to relieve discomfort from overuse. Splints may be recommended as an early treatment to protect and rest sore areas. Anti-inflammatory medicines are often used along with physical therapy like ice packs, ultrasound, or electrical stimulation. Special exercises help tissues move safely while they heal. Assess both your work and recreational activities to figure out if they are adding to your problem. Keep in mind that tension restricts the flow of blood causing muscles and nerves not to get enough oxygen and nutrients, aggravating the symptoms of CTD. Resting the injured area during work and play can relieve tension and allow recovery.
- Relax and pace yourself
- Take breaks often
- Don’t be a stiff when you sit and stand
- Switch up work tasks; Cross train sports activity
- Change or correct your work or play areas
- Avoid caffeine and tobacco
Correct Posture and the Neutral Spine Position
Posture has a big role in CTDs. Slouching the spine or leading with your head puts your body off balance causing your arms and legs to be stretched or bent in awkward positions. The neutral spine position maintains the three natural curves of the spine:
- the inward curve of the neck (cervical) region
- the outward curve of the mid back (thoracic) region
- the inward curve of the lower back (lumbar) region.
Too much curvature or straightening in either the neck or lower back takes the spine out of its neutral position and increases the risk of injury. To prevent injury:
- Instead of leading with your head, rotate the upper body forward at the hips.
- Instead of slouching, rotate your upper body forward at the hips.
- Instead of bending or lifting with a bent lumbar spine, rotate your upper body forward at the hips.
Basic Guide for Sitting Posture
Sitting with a neutral alignment of the spine is also important. Sit in a comfortable chair designed to encourage correct sitting posture. Don’t slouch; sit back in your seat against the back of the chair. Bending your head down strains your neck and affects nerves and arteries that go down into your arms. Relax your shoulders with your elbows, hips and knees bent at a right angle. Avoid pressure to the back of your knees. Keep your feet flat on the floor or support them on a foot rest. Don’t sit still for long periods. Staying in one position causes muscle fatigue and tension. Take breaks often; get up and stretch.
Cumulative Trauma Disorders by Body Area
ElbowLateral EpicondylitisMedial Epicondylitis Radial Tunnel Syndrome Cubital Tunnel Syndrome