The purpose of the following information is to help you understand coronary artery disease (heart disease) and the treatment of it using a coronary stent. If you have any questions about the following information, write them down and discuss them with your doctor, surgeon, or nurse.
About one-third of all Americans develops some form of heart disease. Heart disease is caused by atherosclerosis. Atherosclerosis is a thickening of the inside lining of the blood vessels. This thickening results from the deposit of fatty substances such as cholesterol. As the inside of the blood vessels thicken there is less room for the blood to pass through the arteries. Percutaneous transluminal coronary angioplasty (PTCA or angioplasty) is a procedure that is commonly performed on people with heart disease. This procedure is done to open up the blood vessel to allow the blood to pass through more easily.
PTCA means:
Percutaneous – performed through the skin
Transluminal – through the inside opening of a vessel
Coronary – relating to arteries or veins of the heart
Angioplasty – a procedure to open blood vessels
The common name for PTCA is angioplasty.
Table of Contents
Effects of Heart Disease
What is Angioplasty
Getting Ready
The Procedure
Recovery
Going Home
Medication
Diet & Exercise
Final Word
How does heart disease affect your body?
Your heart is a muscle that needs a constant flow of oxygen-and-nutrient-rich blood to keep it healthy and working properly. Blood reaches your heart through two main coronary blood vessels (arteries). There is also a network of blood vessels covers the surface of the heart and supplies blood to the heart. Fatty deposits and cholesterol can form in your arteries. This results in a narrowing of the arteries, called atherosclerosis.
If your coronary arteries, which supply blood to your heart muscle, become too narrow, they cannot provide your heart with enough oxygenated blood. When your heart beats faster because of physical activity or psychological stress it needs more oxygen and nutrients. Your narrowed or sometimes blocked arteries cannot provide enough blood to the heart. This lack of oxygen can show up as angina (heart pain). In cases of prolonged pain you could have a heart attack. So you can see, it is very important to diagnose and treat heart disease.
When blood fats are too high, it is a lot easier for fat to build up in your arteries. You should know that you are at greater risk for heart disease if you:
- are male
- eat a diet high in cholesterol and fat
- don’t exercise on a regular basis (more than 3 days a week)
- currently have high blood pressure or diabetes
- have a lot of stress in your life
- are a smoker
- are overweight
- have a family member with heart disease
One of the most common tests for finding out if you have heart disease is the stress test (exercise electrocardiogram). You may also hear this test called an exercise treadmill test. This test measures changes in the electrical activity of your heart muscle as you do controlled exercise. The stress test may show if there has been damage to the heart. If the stress test is found to be abnormal, your doctor may want you to have a cardiac catheterization. A cardiac catheterization is the most definitive test for finding heart disease. During the catheterization, a special dye is injected into the coronary arteries. Your doctor will be able to see the dye in the arteries on x-ray pictures shown on a monitor. The x-rays will show any narrowing or blockage in the arteries. After catheterization your doctor will know how much heart disease you have. Your doctor will also know if you need a stent.
What is Angioplasty?
Angioplasty is a surgical procedure that improves blood flow by opening up blood vessels that have narrowed due to deposits of plaque. Angioplasty is done in a cardiac catheterization laboratory (cath lab). The cath lab is an x-ray room with a sterile environment much like that of an operating room. The surgeon makes a small cut usually in the arm or groin. Then a catheter with a tiny balloon on the end is placed into a blood vessel. The doctor then moves the catheter up through the body and into the coronary artery. During this process the doctor will watch the progress of the catheter on x-ray monitors. Once the catheter is placed across the blockage, the doctor slowly inflates the tiny balloon. As the balloon inflates it presses the fatty deposits (called atherosclerotic plaque) against the wall of the blood vessel. By compressing the plaque the inside (diameter) of the blood vessel gets bigger. This bigger vessel makes the blood flow more easily.
However, in about half of all successful angioplasty procedures, the plaque builds up again, causing the inside of the vessel to become smaller, or more narrow. This new build up is known as restenosis. To help reduce the chances of new build up and that narrowing will happen again, your surgeon may suggest placing a coronary stent inside the artery.
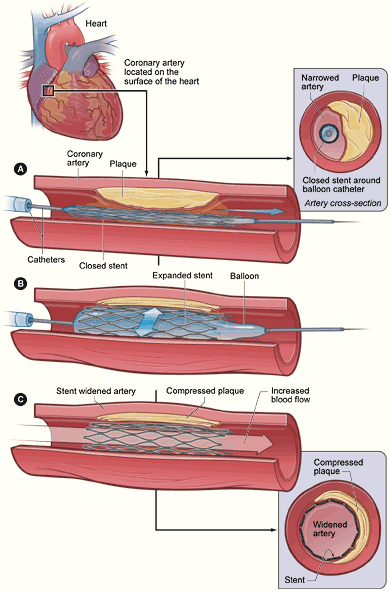
A coronary stent is a small device that provides support for a blood vessel. The stent is a small, stainless steel tube that is placed in your blood vessel. Stents can look like mesh or a small spiral wire (spring). The stent is inserted into the artery by using a balloon catheter after angioplasty. Once in the artery, the surgeon inflates the balloon. As the balloon inflates the stent expands and presses against the artery wall. The balloon is then deflated and removed. However, the stent remains expanded inside the artery and keeps the artery open.
The stent is now a permanent implant that remains in your artery and will help hold the artery open. Since is holds the blood vessel open it also improves blood flow. The improved blood flow should relieve your symptoms of heart disease.
Getting ready for angioplasty and the stent procedure
For several days before the procedure, you will be asked to take aspirin and other medicine given to you by your doctor. Be sure to tell your doctor if you cannot take aspirin for any reason. It is also important to tell your doctor if you are presently taking any medication or if you have any drug allergies. The night before you have the procedure, you will not be allowed to eat or drink anything after midnight.
Before the procedure begins, women will have a urinary catheter inserted into the bladder. Men may have an outside catheter applied. The urinary catheter will reduce the need for moving on and off a bedpan after the procedure. This will minimize stress to the puncture site. Other preoperative instructions will be given to you by your doctor or nurse. You should follow all instructions very carefully.
It is not necessary that you be put to sleep during the procedure. However, you may be given a mild drug to help you relax. The discomfort you feel should be fairly minimal and tolerable. If you need additional pain relief it can be given to you during the procedure. But your doctor will want you to remain as alert as possible so you can follow instructions from him. For example, he will tell you to breathe deeply when x-rays are being taken. Being able to do what the doctor says will improve the quality of the x-ray pictures.
During the angioplasty and stent procedure
 Your procedure will be done in a room that is has special instruments. It will also have a special x-ray machine that has a monitor. The monitor looks like a TV screen and is called a fluoroscope. After you are brought into the room, you will be moved to the x-ray table. You will be covered with a sterile sheet. The place where the catheter is to be placed, usually the inside of your upper leg, will be washed with a special germ killing solution. A local pain-killer will be injected at the site. The pain-killer may sting for a few seconds. Then, a small tube called a sheath will be inserted into the vessel. A smaller plastic tube called a guiding catheter will be passed through the sheath until it gets to the vessels of the heart. A special dye will be injected through the guiding catheter. The dye will show up on the special monitor. The dye allows your doctor to see the veins and arteries in your body.
Your procedure will be done in a room that is has special instruments. It will also have a special x-ray machine that has a monitor. The monitor looks like a TV screen and is called a fluoroscope. After you are brought into the room, you will be moved to the x-ray table. You will be covered with a sterile sheet. The place where the catheter is to be placed, usually the inside of your upper leg, will be washed with a special germ killing solution. A local pain-killer will be injected at the site. The pain-killer may sting for a few seconds. Then, a small tube called a sheath will be inserted into the vessel. A smaller plastic tube called a guiding catheter will be passed through the sheath until it gets to the vessels of the heart. A special dye will be injected through the guiding catheter. The dye will show up on the special monitor. The dye allows your doctor to see the veins and arteries in your body.
The monitor also allows the doctor to see the balloon catheter as it is moved forward through the blood vessel and into the right position. Next, a guide wire will be inserted through the guiding catheter and moved forward to the diseased vessel. Then the balloon catheter will be attached to the guide wire. The balloon will be moved to the site where the vessel is narrowed or blocked. After the balloon catheter has reached the area to be treated the catheter is pulled back a little. This will expose the first balloon. This balloon does not have the stent attached. Then the balloon will be inflated.
As the balloon inflates it applies pressure to the plaque in the vessel. This pressure compresses the plaque and opens the artery. The artery stays open because the plaque is a waxy material and will hold its shape. Once the artery opens up the blood flow increases.
Your doctor will ask you to be very still during this procedure. For the most part you will be comfortable. However, you may experience a feeling of pressure when the balloon is inflated. This feeling is normal and will go away quickly. Once the artery is opened the first balloon catheter will be taken out.
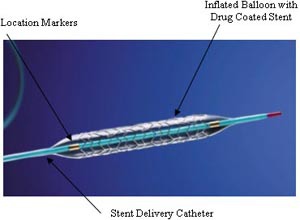
The stent will be mounted on the end of a second balloon catheter. The stent is directed to the area that was previously blocked. The balloon and stent are carefully positioned in the correct spot. The balloon will be inflated causing the stent to expand. One or more stents may be expanded in the vessel. The number of stents you will need depends on the amount of heart disease you have. After all stents are in place, the balloon catheter will then be deflated and removed. The stent remains in place permanently and keeps the coronary artery open. The balloon angioplasty and stent implantation procedure usually lasts between 45 and 90 minutes.
Recovering in the hospital
After the procedure, you will usually be returned to an intermediate cardiac care unit or a medical cardiac care unit. If the sheath is still in place, it will be removed. Pressure will be applied to the puncture site until the bleeding has stopped.
The nurses will watch your heart rhythm and blood pressure very closely. From time to time they will also check your puncture site for bleeding. After a short recovery period, you will be returned to your room. You may eat and drink. Your family will be allowed to visit. Be sure to drink all of the fluids that are given to you. The fluids will help to flush the special dye through your kidneys and out of your body.
For the first few days after receiving your stent, your activities will be restricted. You will be told that you must lie flat until the day after your procedure. You will not be allowed to bend the leg that has the puncture site. A soft restraint may be placed around your ankle. Don’t panic. This is only a gentle reminder that you’re not to move or bend that leg. You must also take medicine that will keep the blood flowing smoothly through your stent. Your blood will be tested frequently to see how quickly a clot will form, called “clotting time”. By monitoring the clotting time the medication dosage can be regulated. Within a few days, your doctor may allow you to gradually increase your activities.
When you go home
Most people who have angioplasty and a stent implant usually stay in the hospital for three to eight days. When the doctor thinks you are ready, you will be discharged to the care of your family doctor. If you have any discomfort, pain, or bleeding of any kind after you get home, you should contact your family doctor or hospital right away.
At first, your doctor will want you to come see him often so he can watch and record your progress. After about six months, your doctor may ask you to have a follow-up stress test or cardiac catheterization. Eventually you will be able to return to your normal activities. Be sure to ask your doctor before you do anything that is physically strenuous.
Your stent will not limit your daily activities in any way. However, you should tell any doctor who treats you in the future that you have a coronary stent. A small wallet-sized card that has additional information about your stent will be given to you by the doctor who implants your stent or the nurse. Remember to keep your stent implant card with you at all times.
Call Your Doctor
Call your doctor if:
- You feel sudden or severe chest pain (angina)
- You have a fever over 101° F
- Pain, swelling, tenderness, redness, or bleeding increases at the incision site
- You have signs of infection (dizziness, fever, muscle aches, headaches)
- You lose sensation in the arm or leg where the blood vessel was used for the catheter
- There are new blue or purple discolorations at the site of the incision
- Your leg or arm feels weak or numb and looks pale or bluish
- The area where the needle was inserted is red, warm, or hot to the touch
- You have a pus-like discharge at the site of the incision
- You have trouble breathing, are short of breath or have pain in your lungs
- You have signs or symptoms of a stroke
If signs tell you it’s an emergency or life-threatening — call 911
Special Medicine
When you get home, you will be instructed to take special medication. Your doctor may also want you to make some lifestyle changes. It takes about 4 weeks for the lining of the vessel to grow over the stent. Once the vessel grows over the stent it will become a permanent part of the vessel wall. Until the blood vessel covers the stent you will be treated with anticoagulants (blood thinners). You will also take an antiplatelet drug. This drug will prevent blood clots from adhering to the surface of your stent until it is covered by your blood vessel. You will be asked to take the following medications for at least one month (the time it takes the blood vessel to grow over the stent). You may have to these drugs longer:
- aspirin for preventing blood clots
- an anticoagulant which also prevents blood clots
- special medication for preventing blood clots
It is very important that you follow the medication regimen exactly as you are told. Do not stop taking any of the prescribed medications unless you are instructed to do so only by the physician who implanted your stent. If you have any side effects from the drugs, such as nausea, vomiting, or rash, you must notify your doctor immediately.
Diet and Exercise
Since angioplasty does not stop fatty buildup in your arteries, your doctor will probably prescribe a controlled exercise program along with lifestyle changes. By changing your diet and exercise, you may be able to get rid of the fatty buildup you already have. If you smoke, you will be encouraged to stop. If your cholesterol is high, you will be taught and encouraged to eat a healthier diet. In addition to following the dietary suggestions from your doctor or dietitian, you should avoid eating too many foods that are high in vitamin K. These foods will decrease the effectiveness of the oral blood thinner that your are taking. The action of a blood thinner can also be affected by antibiotics, some non-prescription medications, vitamins, a change in your eating habits, and especially alcohol consumption. As long as you are taking the anticoagulant, your doctor will probably do a weekly blood test to see how fast your blood is clotting. In the meantime, you should let your doctor know about any lifestyle changes that you make during this time. You should avoid having any dental work while you are taking a blood thinner. If emergency dental work is needed, be sure to tell your dentist that you are taking a blood thinner. You should carefully read over the information packet about the blood thinner given to you by your physician or nurse.
A final word
Because heart disease has been called a “silent disease”, you should have regular periodic examinations to check your progress. Always keep appointments with your doctor. You can reduce your risk of further heart disease by making healthy lifestyle choices.
Keep in mind thousands of people who have heart disease are leading healthy, productive lives after having coronary angioplasty and stent implantation. So can you!