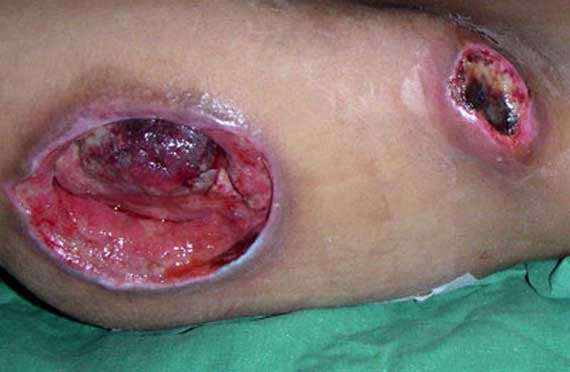
Pressure ulcers, (pressure sores, bedsores, decubitus ulcers) are caused when the muscles and tissues of a particular area of the body presses against a hard surface, like a bed or chair, for prolonged periods. Pressure ulcers are also called bed sores and range in severity from mild (minor skin reddening – Stage I) to severe (deep craters in the skin down to muscle and bone – Stage V). Unrelieved pressure on the skin squeezes tiny blood vessels, which supply the skin with nutrients and oxygen. When the skin is starved of nutrients and oxygen for too long, the tissue dies and a pressure ulcer forms. Skin reddening that disappears after pressure is removed is normal and not a pressure ulcer. Other factors cause pressure ulcers too. If a person slides down in the bed or chair blood vessels can stretch or bend causing pressure ulcers. Even slight rubbing or friction on the skin—called shearing—can cause minor pressure ulcers.
Pressure ulcers are serious problems that can lead to pain, a longer stay in the hospital or nursing home, and slower recovery from health problems. Anyone who must stay in a bed, chair, or wheelchair because of illness or injury can get pressure ulcers. The risk is further increased if the patient is overweight or has no control over their bowels or bladder.
Fortunately, most pressure ulcers can be prevented with close monitoring and proper moving around in a bed or chair. When pressure ulcers do form, they don’t have to get worse.
Where Pressure Ulcers Form
Pressure ulcers form where bone causes the greatest force on the skin and tissue and squeezes them against an outside surface. This can be where bony parts of the body press against other body parts, or a hard surface like a mattress, or chair. In persons who must stay in bed, most pressure ulcers form on the lower back below the waist (tailbone, or sacrum), the hip bone (trochanter), and on the heels of the feet. In people in chairs or wheelchairs, the exact spot where pressure ulcers form depends on the sitting position. Pressure ulcers can also form on the knees, ankles, shoulder blades, back of the head, and spine.
Nerves normally tell us that we are uncomfortable and to reposition our body to relieve pressure on the skin. Persons in bed who are unable to move or can get pressure ulcers after as little as 1-2 hours. Persons who sit in chairs and who cannot move can get pressure ulcers in even less time because the force on the skin is greater from the weight of the body.
Monitoring
Constant monitoring of the whole body by the patient or caregiver is essential in preventing pressure ulcers. Because these sores are predominant in certain parts of the body, these areas should be monitored closely. These areas are:
- Ears
- Back of the head
- Shoulder
- Shoulder blades
- Elbows
- Spine
- Tailbone
- Hips
- Knees
- Heels and ankles
With constant monitoring, you can see the early signs of pressure sores, like redness, warmth, and a hard or spongy feeling area or skin.
Your Risks for Developing a Pressure Ulcer
Confinement to bed or a chair, being unable to move, loss of bowel or bladder control, poor nutrition, and lowered mental awareness are risk factors that increase your chance of getting pressure ulcers. Your risk results from the number and seriousness of the risk factors that apply to you.
- Confined to a bed or chair. If you must stay in bed, a chair, or a wheelchair, the risk of getting a pressure ulcer can be high.
- Inability to move around. If you cannot change positions without help, you are at great risk. Persons who are in a coma or who are paralyzed or who have a hip fracture are at special risk. Risks of getting pressure ulcers are lower when persons can move by themselves.
- Loss of bowel or bladder control. If you cannot keep your skin free of urine, stool, or perspiration, you have a higher risk. These sources of moisture may irritate the skin.
- Not Eating Well. If you cannot eat a balanced diet, your skin may not be properly nourished. Pressure ulcers are more likely to form when skin is not healthy.
- Lowered mental awareness. When mental awareness is lowered, a person cannot act to prevent pressure ulcers. Mental awareness can be affected by health problems, medications, or anesthesia.
Fortunately, you can lower your risks. Following the steps in this article can help you and your health care provider to reduce your risk of pressure ulcers.
Key Steps for Preventing Pressure Ulcers
Pressure sores can be avoided if proper measures are taken with proper skin care, proper clothing and hygiene as well as eating and drinking right. The following preventive measures if followed diligently can keep you away from pressure ulcers.
Take care of your skin
Your skin should be inspected at least once a day. Pay special attention to any reddened areas that remain after you have changed positions and the pressure has been relieved. This inspection can be done by yourself or your caregiver. A mirror can help when looking at hard-to-see areas. Pay special attention to pressure points. The goal is to find and correct problems before pressure ulcers form.
Your skin should be cleaned as soon as it is soiled. A soft cloth or sponge should be used to reduce injury to skin.
Take a bath when needed for comfort or cleanliness. If a daily bath or shower is preferred or necessary, additional measures should be taken to minimize irritation and prevent dry skin. When bathing or showering, warm (not hot) water and a mild soap should be used.
To prevent dry skin:
- Use creams or oils on your skin.
- Avoid cold or dry air.
- Minimize moisture from urine or stool, perspiration, or wound drainage. Often urine leaks can be treated.
When moisture cannot be controlled:
- Pads or briefs that absorb urine and have a quick drying surface that keeps moisture away from the skin should be used.
- A cream or ointment to protect skin from urine, stool, or wound drainage may be helpful.
- Protect your skin from injury
- Avoid massage of your skin over bony parts of the body. Massage may squeeze and damage the tissue under the skin and make you more likely to get pressure ulcers.
Limit pressure over bony parts by changing positions or having your caregiver change your position.
- If you are in bed, your position should be changed at least every 2 hours.
- If you are in a chair, your position should be changed at least every hour. (If you are able to shift your own weight, you should do so every 15 minutes while sitting.)
Reduce friction (rubbing) by making sure you are lifted, rather than dragged, during repositioning. Friction can rub off the top layer of skin and damage blood vessels under the skin. You may be able to help by holding on to a trapeze hanging from an overhead frame. If nurses or others are helping to lift you, bed sheets or lifters can be used. A thin film of cornstarch can be used on the skin to help reduce damage from friction.
Avoid use of donut-shaped (ring) cushions. Donut-shaped cushions can increase your risk of getting a pressure ulcer by reducing blood flow and causing tissue to swell.
If you are confined to bed:
- A special mattress that contains foam, air, gel, or water helps to prevent pressure ulcers. The cost and effectiveness of these products vary greatly. Talk to your health care provider about the best mattress for you.
- The head of the bed should be raised as little and for as short a time as possible if consistent with medical conditions and other restrictions. When the head of the bed is raised more than 30 degrees, your skin may slide over the bed surface, damaging skin and tiny blood vessels.
- Pillows or wedges should be used to keep knees or ankles from touching each other.
- Avoid lying directly on your hip bone (trochanter) when lying on your side.
- Also, a position that spreads weight and pressure more evenly should be chosen — pillows may also help.
- If you are completely immobile, pillows should be put under your legs from mid-calf to ankle to keep heels off the bed. Never place pillows behind the knee.
If you are in a chair or wheelchair:
- Foam, gel, or air cushions should be used to relieve pressure. Ask your health care provider which is best for you. Avoid donut-shape cushions because they reduce blood flow and cause tissue to swell, which can increase your risk of getting a pressure ulcer.
- Avoid sitting without moving or being moved.
- Good posture and comfort are important.
A doctor or a healthcare provider should be contacted immediately at the very early signs of redness, bruise, cut, sore, or any other skin changes, and also if your wheelchair does not fit properly.
Eat well
Eat a balanced diet. Protein and calories are very important. Healthy skin is less likely to be damaged by pressure.
If you are unable to eat a normal diet, talk to your health care provider about nutritional supplements that may be desirable.
Improve your ability to move.
A rehabilitation program can help some persons regain movement and independence.
Be Active in Your Care
This information tells how to reduce your risk of getting pressure ulcers. Not all steps apply to every person at risk. The best program for preventing pressure ulcers will consider what you want and be based on your condition.
Be sure you:
- Ask questions.
- Explain your needs, wants, and concerns.
- Understand what and why things are being done.
- Know what is best for you. Talk about what you can do to help prevent pressure ulcers — at home, in the hospital, or in the nursing home.
You can help to prevent most pressure ulcers. The extra effort can mean better health.
[adsense_id=”1″]